Building Middleware for Healthcare: Connecting Robotics, ERP, and National HIS
Healthcare automation rarely fails because of hardware. It fails because systems don’t talk to each other.
This case explores how SDH designed and deployed a middleware architecture that connected a pharmacy robot, an ERP platform, and a restricted national Health Information System (HIS). The result: fully automated medication workflows, real-time visibility, and a scalable model ready for national rollout.
For organizations responsible for technology strategy and growth partnerships, this project demonstrates what it takes to integrate regulated healthcare platforms and build infrastructure that scales beyond a single hospital.
The Integration Challenge: Three Systems, One Workflow
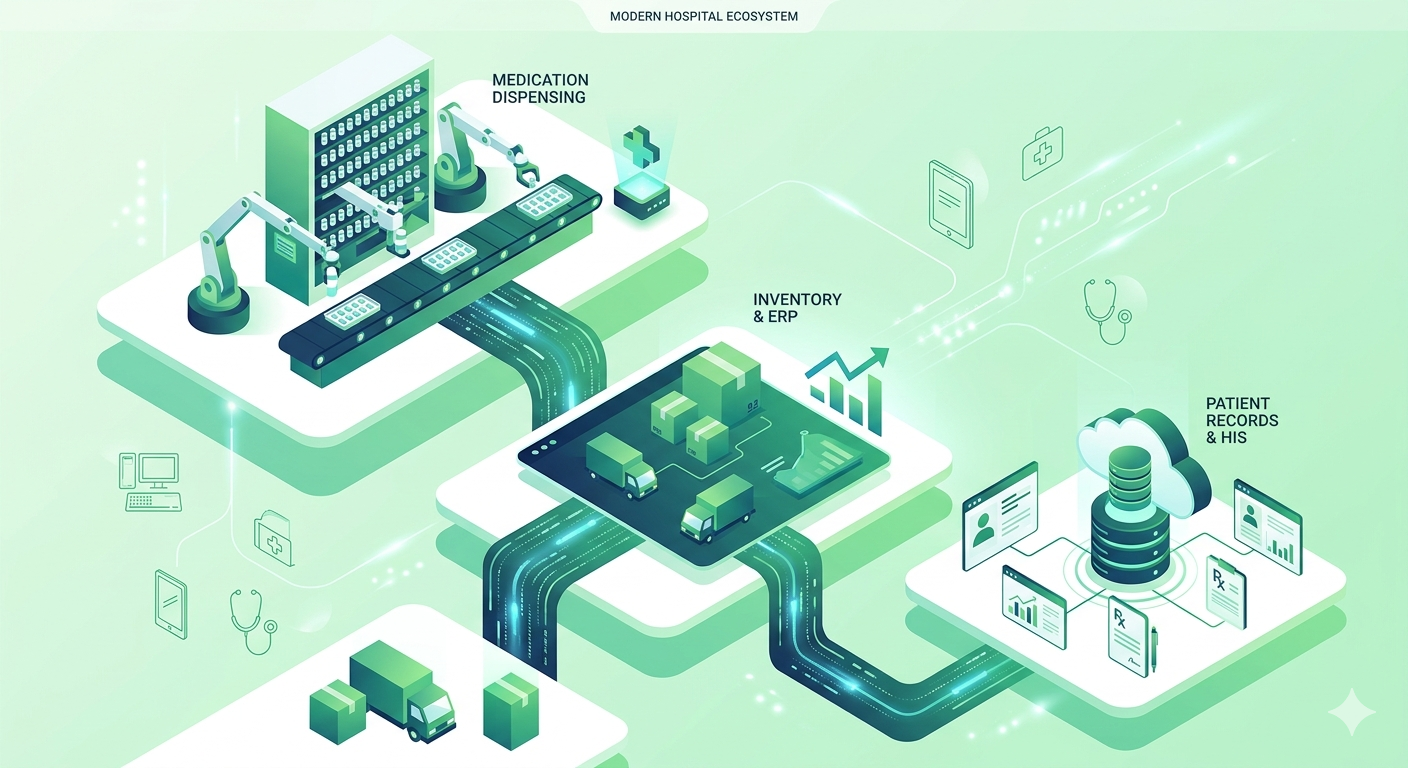
Modern hospitals rely on multiple specialized systems:
- Robotics to store and dispense medications
- ERP systems to manage inventory, procurement, and accounting
- National HIS platforms to store patient records and clinical orders
Individually, these systems work well. Together, they often create operational friction.
In this case, a hospital deployed a pharmacy automation robot designed to store, retrieve, and dispense medications with high precision. However, without live synchronization with hospital ordering and record systems, staff still had to manually bridge the workflow between systems.
Manual intervention introduced:
- Increased risk of medication errors
- Workflow delays
- Inconsistent inventory records
- Reduced ROI from automation hardware
The technical barrier was even more significant than the workflow gap.
This meant traditional integration approaches weren’t enough.
The Strategic Decision: Build a Middleware Layer
Instead of attempting direct, one-off connections between systems, SDH implemented a centralized middleware architecture.
The goal was not simply integration—but system orchestration.
Core Objectives
- Connect robotics, ERP, and national HIS systems
- Enable real-time data exchange
- Automate medication lifecycle workflows
- Maintain compliance with national healthcare standards
- Build an architecture ready for multi-hospital deployment
This required both technical engineering and collaborative governance with national system stakeholders.
The Middleware Architecture
The resulting system introduced a middleware layer positioned between all three systems.
Instead of connecting each component directly to every other component, the middleware became the central communication hub.
System Flow Overview
- A clinician submits a medication order in the HIS
- The middleware captures the request
- The robot receives instructions and dispenses medication
- The ERP records inventory and transaction details
- The middleware synchronizes status updates across all systems
Every step happens automatically.
No duplicate data entry.
No manual reconciliation.
No workflow gaps.
This design delivered full end-to-end automation of the dispensing lifecycle.
Real-Time Visibility: The Dashboard Layer
Automation alone is not enough. Visibility is equally critical.
The solution included a live operational dashboard that provided pharmacy managers with real-time insights across the workflow.
Key dashboard features included:
- Medication dispensing status
- Inventory movement tracking
- Order lifecycle visibility
- Exception alerts
- Performance metrics
This visibility transformed pharmacy operations from reactive to proactive.
Managers could identify delays, track trends, and maintain full operational awareness.
Engineering for Scalability from Day One
Many integrations work only at a single-site level. Scaling them often requires rewriting the architecture.
This system was designed differently.
From the beginning, the middleware supported:
- Multi-hospital deployment
- Multiple device types
- Future robotics integrations
- Additional ERP modules
- Expansion into new facilities
New systems could plug into the existing infrastructure without redesigning the core.
That scalability decision proved critical.
After initial deployment, the solution was successfully adopted across public hospitals, with national expansion underway.
Delivery Metrics and Timeline
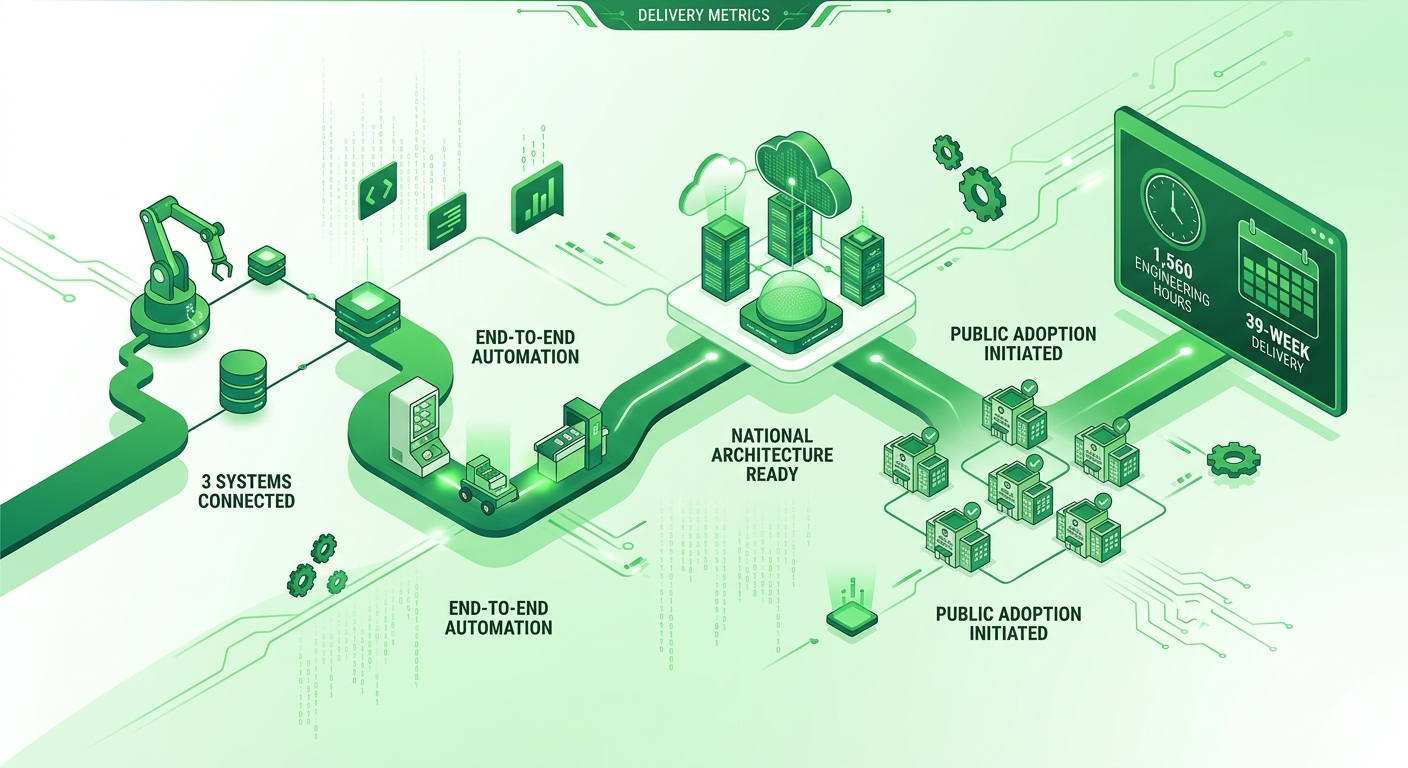
The implementation was not only technically complex—it was also tightly structured.
Key delivery metrics included:
- 3 systems fully connected, including a restricted national HIS
- End-to-end dispensing lifecycle automated
- National-level architecture readiness achieved
- Adoption across public hospitals initiated
- 1,560 engineering hours invested
- 39-week delivery timeline completed
These numbers reflect not just development time—but regulatory alignment, testing cycles, and production readiness.
Business Impact Beyond IT Integration
This project created measurable operational and strategic value.
Operational Gains
- Reduced manual handling of medication workflows
- Improved accuracy and patient safety
- Faster dispensing cycles
- Real-time synchronization across systems
Strategic Gains
- Increased ROI from automation hardware
- Improved readiness for national healthcare digitization
- Standardized integration framework
- Reduced future onboarding costs
For healthcare organizations planning modernization, these outcomes represent multiplicative value, not incremental improvement.
Why Middleware Matters in Healthcare Modernization
Healthcare environments are evolving toward interconnected digital ecosystems.
Robotics, AI tools, ERP systems, and national platforms must function as a unified infrastructure.
Middleware is what makes that possible.
Without middleware:
- Systems remain isolated
- Automation remains partial
- Scaling becomes expensive
- Data accuracy declines
With middleware:
- Systems become modular
- Workflows become automated
- Infrastructure becomes reusable
- Innovation becomes scalable
This architectural shift is especially important in regulated industries where system interoperability is mandatory.
Lessons Learned from the Integration
Several strategic insights emerged from the implementation.
1. Integration Requires Partnership, Not Just Development
Working with national HIS stakeholders was as important as writing code.
Successful integration often depends on collaborative governance, not just APIs.
2. Scalability Must Be Designed Early
Retrofitting scalability later is expensive.
Designing reusable integration patterns from the start reduces long-term costs.
3. Middleware Enables Vendor Neutrality
By abstracting integrations into middleware, hospitals can adopt new robotics or ERP systems without rebuilding their ecosystem.
This flexibility protects long-term investment value.
4. Visibility Drives Adoption
Operational dashboards increased confidence in automation and accelerated adoption across facilities.
Transparency builds trust.
A Blueprint for National Healthcare Integration
The architecture delivered by SDH is more than a single integration.
It represents a repeatable model for healthcare modernization.
As healthcare systems expand automation programs, they face similar challenges:
- Connecting robotics platforms
- Synchronizing enterprise systems
- Integrating national healthcare platforms
- Scaling infrastructure across facilities
Middleware-centered architecture provides a clear solution path.
Final Thoughts: Integration as a Competitive Capability

Healthcare innovation increasingly depends on connectivity.
Robotics alone doesn’t transform healthcare.
ERP systems alone don’t improve workflows.
National HIS platforms alone don’t create automation.
Integration does.
By building a middleware ecosystem that connects robotics, ERP, and national health systems, SDH delivered more than technical infrastructure - they delivered a scalable digital backbone for healthcare operations.
For organizations responsible for technology architecture and strategic partnerships, this case illustrates a critical reality:
Healthcare modernization is no longer about systems - it’s about ecosystems.
Categories
About the author
Share
Need a project estimate?
Drop us a line, and we provide you with a qualified consultation.





